Pain that originates from the back of the foot or caudal heel pain.
Recently, the definition of ‘heel soreness’ or ‘navicular syndrome’ in horses has been thrown on its head. With new developments in diagnostic tools for horses, it has become obvious that there are many causes of this syndrome.
We used to think that heel soreness originated from pain in the navicular bone. We never really knew the etiology (cascade of events) for the pain. But, now with diagnostics like MRI, we are finding that the reasons are more numerous than we could have imagined.
Clinical Signs
Most horses present to the clinic with a gradual onset, progressive forelimb lameness that often appears to move from one front foot to the other. There may be one foot that is more lame than the other, and with time that hoof will become smaller than the opposite hoof. The lameness may be exacerbated by trotting on hard surfaces, and in tight circles. The horse oftentimes shows more lameness when the most lame limb is on the inside of the circle. Hoof testors can be used to evaluate for tenderness in the heel/navicular area. But, the lack of hoof tester sensitivity does not rule-out a diagnosis of navicular syndrome.
The most common breeds are quarter horses and thoroughbreds, with the highest incidence between the ages of 7 and 14; however, any breed can be affected.
Diagnosis
We always start with a thorough lameness exam to characterize the lameness and localize the area of pain. Nerve blocks are used to methodically “numb out” areas of the foot and limb. Most of the time, we start with a palmar digital nerve block (PDN). By injecting a small amount of carbocaine (a local anesthetic) around the palmar digital nerves, the heel area can be desensitized or “numbed out”. If the horse then trots sound on that limb, we know the origin of pain is coming from the area that was “numbed out”. Most of these horses will then show lameness in the opposite limb. We assume that this block only affects the structures in the heel area, or back half of the foot, but we would be wrong. The PDN block is much more unpredictable than we once thought. Scientific studies and our own experience shows injuries to structures in the area of the pastern or fetlock have been affectively blocked with the PDN block.
Once we have established that a PDN block eliminates the lameness, the next step is to take radiographs or x-rays of the feet and pastern areas. These radiographs will show some changes in the bones, but are not sensitive enough to show all bony abnormalities. There are some characteristic changes to the navicular bone that we can see on radiographs. Changes like increased numbers or size of the vascular channels within the bone, increases in the density of the inside of the navicular bone, or some erosions on the surface of the bone, can be seen. All these indicate abnormal stresses on the navicular bone, causing the bone to modify its structure.
Not too many years ago we used to just stop here and treat the horse for navicular syndrome. But, now with the knowledge that these horses can have multiple problems/injuries, further diagnostics are warranted. Ultrasound, nuclear scintigraphy, CT and MRI can all be used to discover or rule-out other problems in the area of the foot, pastern, and fetlock.
It is also important to remember that not all horses with clinical signs of navicular syndrome have changes on radiographs. When a patient’s lameness blocks with the PDN block, and there are no radiographic abnormalities, then secondary imaging is indicated. Ultrasound can be used to evaluate the soft tissue structures of the pastern and fetlock area, but can not ‘see thru’ the hoof wall to view the soft tissue structures of the foot. Nuclear scintigraphy can show where there are areas of bone inflammation, but can not tell us what the inflammation is from.
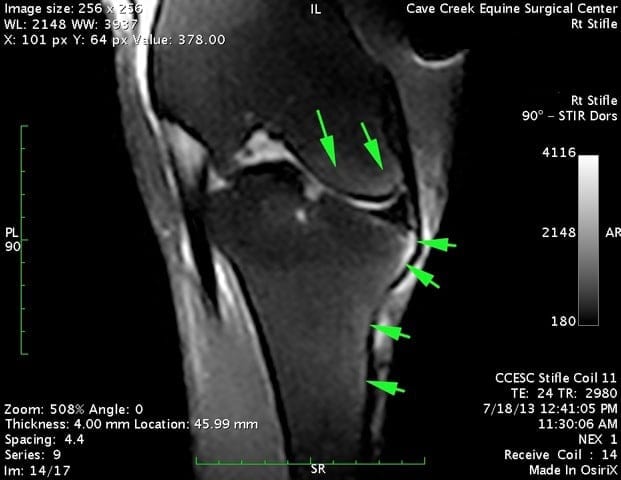
One of the most important advances in the diagnosis of foot/heel pain is MRI. With MRI, both the bones and the soft tissues can be evaluated in terms of their structure and physiology. Certain MRI protocols can show fluid build-up within a structure than can indicate inflammation, or increased density of a bone indicating chronic stress to that area. The list of differential diagnoses has grown due to the detailed evaluation of both bone and soft tissue structures by MRI. We now understand why there can be such a discrepancy between lameness and the radiographic appearance of the navicular bone.
Once the MRI scan is performed and the hundreds of images evaluated by an experienced radiologist, then treatment recommendations can be made.
Types of problems that can cause the signs of navicular syndrome:
Navicular bone
- osteonecrosis
- edema
- fibrocartilage erosions
- suspensory ligament injuries
- fragmentation/avulsion of the distal tip of the bone
- impar ligament injuries
- navicular bursitis
- bony stress fractures
Deep digital flexor tendon
- tendon fraying
- tendon tears
- adhesion to the navicular bone
Coffin joint
Coffin bone/lamina
- edema
- laminitis
- keratoma
- chondrocoronal ligament injuries
- bony stress fractures
Pastern area
- straight, oblique or cruciate distal sesamoidean ligament injuries
- inter-sesamoidean ligament injuries
- superficial digital flexor tendon injuries
- pastern joint arthritis
- deep digital flexor tendon injuries
- bony stress fractures
Fetlock area
- fetlock collateral ligament injuries
- suspensory branch injuries
- joint cartilage damage
- bony stress fractures
In our experience, there is often more than one injury/problem discovered. In order to reliably treat the lameness, all injuries need to be identified and treated. Thinking, “that injury is too high in the lower limb to be causing the lameness; the PDN block does not go that high” can be a big mistake. Injuries to the suspensory ligament branches (just above the fetlock) have been identified as the cause of lamenesses that blocked out with a PDN block.
Treatment
Treatment can now be tailored to each individual injury. It is very important for the success of the treatment, that all injuries are addressed and treated. Some may need to be re-treated at a later date.
Here is a list of just some of the treatment options:
Systemic treatment
- isoxsuprine- vasodilator that increases blood flow to the foot
- antiinflammatories- NSAIDS like bute and banamine
- tildren- bone modulator. Promotes bone repair.
- adipose Derived Stem Cells- healing and repai
- pergolide- treats Cushings Sydrome which can help control laminitis. Also used for treating laminitis associated with Insulin Resistance.
Local treatment
- adipose Derived Stem Cells- healing and repair
- IRAP-(interleukin 1 receptor antagonist protein), anti-inflammatory, growth factors
- PRP- platelet rich plasma- healing and repair
- corticosteroid injection of joints/bursa- anti-inflammatory
- shockwave therapy- increase blood flow, anti-inflammatory
Other
- Corrective trimming and shoeing- heel support, shock absorption, and improved breakover
- Neurectomy
- Bursoscopy- surgical scoping of the navicular bursa
- Rest with controlled rehabilitation
Regular monitoring of the healing process is also important to determine if re-treatment or an alteration in the rehabilitation program is required. This monitoring may consist of examination, x-rays, ultrasound, or MRI.
Prognosis
With an accurate diagnosis and specific treatment, the majority of horses with ‘foot/heel pain’ regain soundness. We have also noted a dramatic decrease in the numbers of horses that require neurectomy to become sound. Which supports the idea that “by indentifying and treating all of the injuries individually, we can actually repair most of the damage instead of just masking the pain”. Many horses with ‘foot/heel soreness’ return to their normal activity levels.